Anaphylaxis Causes and Risk Factors: What You Need to Know

Anaphylactic allergy reactions can be intense and life-threatening. They can occur within minutes or even seconds of exposure and each person’s body reacts differently. Anaphylaxis is dangerous, but knowing how to recognize it and taking critical steps to get help can make all the difference. Whether your reaction is caused by food allergies, bee stings, medicines, or other substances, it’s important you take precautions to prevent these reactions and make a plan to deal with any future instances of anaphylaxis.
What Is Anaphylaxis?
Anaphylaxis is a severe, potentially life-threatening allergic reaction that can be triggered by exposure to particular allergens or irritants. When the body’s immune system senses an extreme threat it floods the body with chemicals that can cause anaphylactic shock, often appearing in the form of swelling, difficulty breathing, increased heart rate, and other serious symptoms.
An anaphylactic reaction is most commonly triggered by an allergy to foods, drugs, latex or insect stings, but there are other rare causes and conditions as well. If you experience anaphylactic shock it is important to use an epinephrine pen if possible and then seek medical help at a hospital right away. It’s essential to determine what allergies triggered your reaction so you can prevent and prepare for any severe allergic reactions in the future. If anaphylaxis isn’t treated quickly, it can cause permanent damage or even be fatal.
Symptoms of Anaphylaxis
 Recognizing the early symptoms of anaphylaxis can allow you to get help as soon as possible, before your body enters more severe anaphylactic shock. Earlier symptoms may start within seconds of exposure or may be more delayed, but either way they should not be ignored.
Recognizing the early symptoms of anaphylaxis can allow you to get help as soon as possible, before your body enters more severe anaphylactic shock. Earlier symptoms may start within seconds of exposure or may be more delayed, but either way they should not be ignored.
Early symptoms of anaphylaxis can include:
- Tingling hands, feet, mouth, or scalp
- Itchy skin, hives, or flushed skin
- Suddenly feeling too warm
- Wheezing or difficulty breathing
- Chest tightness or discomfort
- A week or rapid pulse
- Swollen tongue or lips
- Cough
- Runny nose and sneezing
- Nausea or vomiting
- Abdominal pain
- Difficulty swallowing or lump in your throat
- Slurred speech
- Confusion or fogginess
More severe symptoms that could be a sign of progression into anaphylactic shock may include:
- Low blood pressure (hypotension)
- Weakness or dizziness
- Fainting or unconsciousness
- Abnormal heart rhythms
- Rapid pulse
- Loss of oxygen
- Extreme difficulty breathing
- Blocked airways
- Hives
- Severe swelling of the eyes, face, or affected body part
- Shock
- Cardiac arrest
- Respiratory arrest
The sooner you can receive medical attention for anaphylaxis symptoms, the better. An anaphylactic reaction always requires a visit to the emergency room, even after an EpiPen has been used, and even if symptoms don’t appear immediately serious.
Causes and Triggers of Anaphylaxis
There are many different irritants or allergens that can trigger an anaphylactic reaction. If it is unclear what is causing your allergy attacks, an in-office allergy test or at-home test kit can determine exactly what you are allergic to.
Allergens that commonly trigger anaphylaxis include:
Foods
While anaphylaxis can occur with any food allergy, certain foods are more commonly known to cause this severe reaction. Peanuts, tree nuts, fish, shellfish, milk, and eggs are some of the most frequent triggers of anaphylaxis due to food allergies. Reading food labels and asking about ingredients when eating out is extremely important for anyone diagnosed with food allergies that could cause an anaphylactic reaction.
Insect Venom
Insect stings and bites are a common cause of anaphylaxis in both children and adults. The insects that cause these reactions include yellow jackets, honey bees, paper wasps, hornets and fire ants. Since exposure to these insects often occurs outside, away from medical aid, it’s important for those with insect venom allergies to carry an EpiPen for outdoor activities such as hiking, bike riding, etc. If you’ve never been stung before but have had anaphylactic reactions to other substances, there is a higher likelihood you will experience anaphylaxis after an insect sting.
Medications
Medication allergies are another common cause of anaphylactic reactions for patients of all ages. Drugs that most frequently cause severe allergic reactions include penicillin, aspirin, and over the counter (OTC) anti-inflammatory drugs like Advil (ibuprofen) and Aleve (naproxen).
Anaphylaxis can occasionally occur as a result of a patient’s exposure to general anesthesia, contrast dyes for imaging studies, certain opioids, and monoclonal antibodies, usually through intravenous (IV) administration. While less common, medication-induced anaphylaxis can also be triggered by insulin, sulfa drugs, antibiotics, oral anesthetics, and some drugs used to treat seizures.
Latex
Latex is a natural rubber product that has been used in many items since the 1980s. While the latex gloves produced today don’t contain nearly the amount of allergy-causing proteins found in these gloves in the past, certain people’s sensitivities are still strong enough that they can be instantly affected by exposure to latex gloves or balloons.
Exercise
A rare cause of anaphylaxis called exercise-induced anaphylaxis (EIA) can result from physical activity. The triggering exercise can be anything from jogging to swimming or even strenuous household chores, but also typically involves another trigger such as foods, medications, or extreme temperatures. Symptoms include tiredness, warmth, itching, and redness, usually within a few minutes of starting exercise.
Dust Mites
Another rare allergy that can cause anaphylaxis is dust mites, often as a result of eating foods that were contaminated with dust mite particles. This is called oral mite anaphylaxis (OMA), or pancake syndrome. Dust mites are a common cause of allergies, but they are usually found in bedding, carpeting, or other fabrics. However, they can also contaminate food products such as flour and other cereal grains, which may lead to an anaphylactic reaction within minutes of ingesting if someone has this allergy.
Red Meat
A rare type of anaphylaxis can happen to people who were bitten by a tick that recently fed on blood from farm animals. These patients can become sensitive to the alpha-gal carbohydrate which can be found in the meat from all mammals (beef, pork, lamb, and goat). This causes them to have a severe, but often delayed, allergic reaction when they eat red meat.
Risk Factors for Anaphylaxis
There aren’t many controllable risk factors that can predict or worsen anaphylaxis. However, there are still a few risk factors that can affect the likelihood of experiencing an anaphylactic reaction, as well as the type and severity of anaphylaxis.
Risk factors for severe anaphylaxis include:
Previous Anaphylactic Reactions
If you’ve previously suffered from anaphylaxis before, your risk of having this serious reaction increases. Future reactions might be more severe than the first reaction, and new triggers may emerge after an initial anaphylactic reaction.
Allergies or Asthma
People who already have seasonal or year-round allergies are at increased risk of experiencing anaphylaxis, as are patients who have asthma. Even people with mild asthma are at a higher risk for severe allergic reactions. Pre-existing conditions like allergies and asthma already affect breathing and can make you more likely to have severe issues with airway constriction and oxygen loss during an anaphylactic episode.
Family History of Anaphylaxis (Genetics)
Allergies tend to run in the family and there is believed to be a genetic predisposition to allergies and asthma alike. People with family members who have allergies to common anaphylactic triggers are likely more at risk. It’s important to realize you could also develop anaphylaxis at any stage in life, even if prior exposures to the allergen did not affect you.
Cardiovascular
If you have a cardiovascular disease that is not under control you may be at a higher risk of death due to anaphylaxis. People with cardiovascular disease who are taking beta-blockers or alpha-adrenergic blockers are at further risk if they develop anaphylaxis since these medications reduce the effects of epinephrine, which is the best treatment that can be given to stop the severe reaction.
Complications of Anaphylactic Shock
Anaphylaxis can be life-threatening. A severe reaction can stop your breathing and even your heartbeat, so it’s important to receive medical attention as soon as possible after exposure. During and after an anaphylactic reaction it is possible to experience complications caused by the body’s chain reaction response to allergens. A decrease in blood pressure is common which can prevent the heart and brain from getting enough oxygen.
Potential complications that can be caused by anaphylaxis include:
- brain damage
- kidney failure
- cardiogenic shock
- arrhythmias, (heartbeat that is too fast or too slow)
- cardiac arrest
- lung damage
- death
- worsening of pre-existing medical conditions
The sooner you are treated for anaphylactic shock, the fewer complications you’re likely to experience.
What to Do in Case of Anaphylactic Shock
If you are experiencing anaphylaxis, take the following steps:
-
Stay Calm and Find Help
If you are experiencing a severe allergic reaction like anaphylaxis, it is important to remain calm and stay focused. Anxiety and panic can make symptoms worse and cause them to happen faster. If you are alone, call 9-1-1 immediately. If you are with someone, explain in detail what just happened, what you think the allergen trigger is, what your symptoms are, and if you have a history of anaphylaxis. You may start to feel foggy and disoriented quickly, so it’s important to communicate as quickly as possible with someone who can help.
If you are helping someone who is experiencing anaphylaxis, encourage them to stay calm and breathe as smoothly as possible.
-
Get Emergency Medical Care Immediately
Always go to the hospital or emergency room when experiencing an anaphylactic reaction. Even after injecting epinephrine, it is important to have a doctor monitor your condition and administer any further medications needed such as additional epinephrine, antihistamines, and corticosteroids. Whether this means driving to the nearest clinic right away or dialing 9-1-1 to have an ambulance come for the quickest treatment, seek medical attention as soon as possible. Minutes or even seconds can make all the difference during a severe allergic reaction.
Anaphylaxis symptoms can come back even several hours after the initial exposure, so it’s important to be monitored and treated for some time. The possibility of cardiac or respiratory complications that need treatment is higher for people over the age of 50 or with preexisting conditions.
-
Use an EpiPen if Possible
If you have a prescription epinephrine auto-injector (EpiPen or Auvi-Q), use it at the first sign of symptoms. Inject yourself if you are able to do so, or ask someone else to read the instructions carefully and then administer the injector. A single injection of epinephrine may not be enough to stop anaphylaxis.
If severe symptoms continue an additional dose can be given after five to ten minutes. Emergency responders may also be able to administer epinephrine when they arrive, but this is one of the reasons it is so important to get to emergency medical assistance quickly.
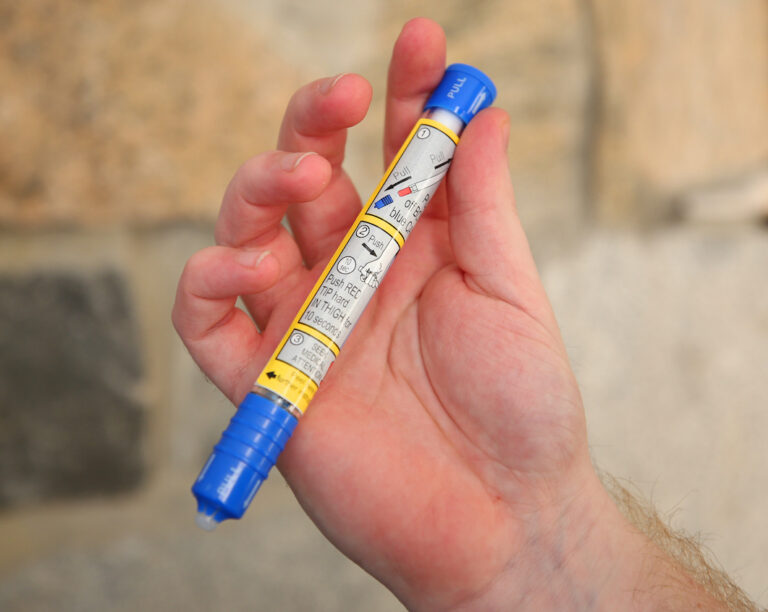
How to use an EpiPen –
- Be careful not to hold the injector backwards, which can stick the needle into your thumb instead of your thigh. This is a common mistake and a bigger issue if the person using the EpiPen is not the one having a reaction.
- Pull the blue safety cap off the back of the device.
- Press the orange end firmly into the thigh and hold it for at least 3 seconds. It works best to administer the shot directly to the skin, but injecting through clothing is fine if necessary.
- Needle protection is built in and will automatically be covered after injection so it is never exposed and easily disposed of afterward.
How to use an Auvi-Q –
The Auvi-Q is a rectangular device around the size of a credit card that uses a series of voice prompts to provide step-by-step instructions on using it correctly and preventing accidental needle sticks. Follow the instructions carefully to successfully administer the epinephrine injection.
Do not try to take any oral allergy medications if you have started experiencing trouble breathing. This will not be effective quickly enough and you need to use an epinephrine injector and seek medical attention right away instead.
-
Remove the Allergen
If the trigger causing the allergic reaction is a food allergy, be sure to remove any remnants of the food from the mouth and throat, and/or remove the person from the area of exposure. If the allergen is topical, such as poison ivy or a medical ointment, wash the skin off as thoroughly as possible.
If anaphylaxis is being caused by an insect sting, remove the stinger as soon as possible. The longer the stinger remains in the skin, the worse the reaction will likely be. Take care not to squeeze the stinger as you remove it, as this could inject even more venom. Instead, use a plastic card such as a credit card. Press the card against the skin, slide toward the stinger at an upward angle, and flick the card up once it is underneath the stinger.
-
Call 9-1-1 for Anaphylactic Shock
If the allergic person has progressed into severe symptoms such as trouble breathing, they are likely going into anaphylactic shock. If you haven’t already called 9-1-1 do so immediately, even if an epinephrine injection has already been given.
-
Monitor Symptoms While Waiting for Emergency Responders
The allergic person should lay down and elevate their legs while waiting for emergency responders. This helps to keep blood flow going to the heart during an anaphylactic reaction. If they do not feel comfortable laying down because of vomiting or difficulty breathing, have them sit comfortably and still elevate the legs if possible. Monitor the person’s pulse and breathing so you can give an accurate update when medical help arrives, and give CPR if necessary.
How to Treat Anaphylaxis
The only truly effective treatment for anaphylaxis is Epinephrine. This shot of adrenaline will always be the first treatment administered by medical professionals, and may even be injected before medical help arrives if the person is prescribed an auto-injector EpiPen. This injection can reduce the severity of the allergic reaction, but more than one dose will likely be needed which is why a hospital visit is a must.
Once at the hospital, doctors and specialists can appropriately monitor you and provide treatments as needed. In addition to epinephrine, it’s possible you may be given oxygen, IV fluids, IV antihistamines, corticosteroids, and a beta-agonist such as albuterol to help with breathing and reduce the allergic response. These medications reduce inflammation and help reopen the air passages. If breathing is blocked entirely a breathing tube can be put down the throat (intubation) or an emergency surgical airway (cricothyroidotomy) can take place in the neck to get air into your lungs.
Any complications that have occurred as a result of anaphylactic shock will also be treated at the hospital or urgent care.
How to Prevent Anaphylaxis
The best way to prevent an anaphylactic reaction is to avoid the allergens or substances that cause this severe reaction. This is easier to do for some than for others, depending on the irritant or trigger.
In addition to avoiding known triggers, there are several other ways to prepare yourself and prevent the worst in the event that anaphylaxis occurs.
- If you are allergic to certain foods, it’s important to carefully read the labels of all the foods you buy and eat. Manufacturing processes can change, so check periodically on the foods you commonly eat to make sure it does not contain your allergen. Always ask for details on ingredients and preparation when eating out at restaurants. Watch out for foods that may be included as ingredients in other non-food items, such as coconut or tree nuts used in shampoo.
- Wear a medical alert bracelet or necklace which indicates your specific allergies. This can help others understand what may be happening to you if you’re experiencing anaphylactic shock, and could save your life if you are unable to respond when help arrives.
- Keep an emergency med kit with prescribed medications and autoinjectors (EpiPen) in your car or on your person at all times. If you have an epinephrine auto-injector, be sure to consistently check the expiration date and refill the prescription before it expires.
- Use caution in areas where they are likely to be stinging insects. If you know you’re allergic to insect stings, wear long-sleeves, pants, and closed shoes outdoors, avoid walking barefoot on grass, dress without bright colors, and make sure not to wear perfumes, colognes or scented lotions as these can attract bees and wasps. Don’t drink from open cans or containers when outdoors. If approached by a stinging insect calmly move away instead of swatting at the insect.
- Create a plan with your doctor and be prepared. An allergy response plan will help you learn to pay attention and prepare for anaphylaxis in a number of situations. It will also help you educate others in your life about the allergy and what to do in case of a severe reaction. Review this plan with your doctor and family each year to make and necessary changes.
What to Expect After Anaphylactic Shock
Anaphylaxis is extremely dangerous and can cause serious damage or be fatal if you don’t receive immediate medical attention. Your recovery process will likely depend on how quickly you get help.
Complications are common as a result of anaphylactic shock, especially for people over 50 years of age or who have existing cardiac or respiratory issues. These complications will need to be addressed, diagnosed and treated on an individual basis by medical professionals.
A doctor or ENT specialist will work to determine the allergen or trigger which caused your reaction, if still undetermined. They will likely conduct an allergy test to get a complete picture of all allergies you may have and how severe they may be. After determining allergies you may be prescribed allergy medications such as oral pills or allergy drops to reduce the likelihood and severity of future allergic reactions. You may also be prescribed an EpiPen to be prepared for an epinephrine injection in case of another anaphylaxis attack.
Take Action to Prevent and Prepare for Anaphylaxis
Immediate action is everything when it comes to anaphylaxis. If you or someone close to you experiences an anaphylactic reaction it’s important to remain calm, seek medical help right away, use an EpiPen if possible, and get to a hospital for continued monitoring. Work with your doctor and ENT specialist to determine your exact allergies, make a plan for prevention, and prepare for any future anaphylactic episodes. If you are concerned about allergic reactions and want to understand your allergies, consult with an expert ENT doctor today.

